
Lauren Beasley – contributing writer for Breaking Muscle!
Some things just go together. Peanut butter and jelly. Jordan and Pippen. Cheech and Chong. You could have one without the other, but things just wouldn’t be the same. In the body, arguably the biggest power couple is the ball and socket – a term synonymous with the shoulder. But in the body we don’t just have great duos, we have amazing kinetic chains. PB&J would never have made it big without the bread (pre-paleo). Phil Jackson was the one who merged two megastar individual talents into the synergistic backbone of the Chicago Bull legacy. And Cheech and Chong? Well, we all know what their magic ingredient was.
My Shoulder Has a Complex
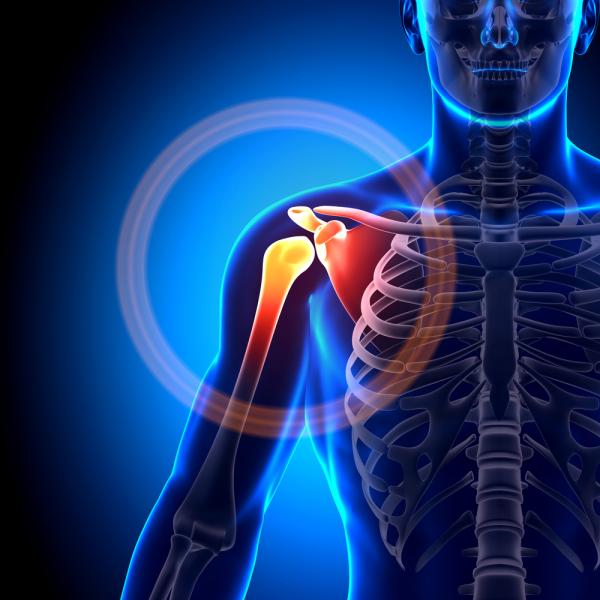
While the term “shoulder” most commonly refers to the ball and socket mechanism, the shoulder complex actually consists of multiple joints:
 The first, and only “hard” connection between our arms and axial skeleton (skull, spine, ribcage, and sternum) is the costoclavicular joint, or where the collarbone meets the sternum.
The first, and only “hard” connection between our arms and axial skeleton (skull, spine, ribcage, and sternum) is the costoclavicular joint, or where the collarbone meets the sternum.- Following the clavicle away from midline – distally – the next union is our acromioclavicular joint (AC). Here the clavicle sits on top of a projection from the scapula called the acromion process. When the shoulder is “separated,” this is where that dislocation occurs.
- No introduction is necessary for the next joint in line, the ball and socket, or glenohumeral joint (GHJ).
- Although not technically a real joint, the final articulation in the shoulder complex is the scapulothoracic joint (STJ), or the “connection” between the shoulder blade and the thoracic spine and associated ribs.
Together, this intricate cluster of joints creates the incredible shoulder – the cornerstone of movement through the upper extremity. But like any great team, many do the work while few get the credit. Ask Jordan or Pippen.
The Roles of the Joints in the Shoulder Complex
 The glenohumeral joint is the MVP of our shoulder complex. It’s flashy, makes the big plays, and scores all the points. The GHJ joint is the single most mobile joint in the body. But, thanks to the laws of physics, mobility exists at the expense of stability. Picture a golf tee and a golf ball – this is the age-old analogy that best describes the dimensions of the GHJ joint. When the tee is set just right, the ball can sit perfectly centered in the shallow support of the tee. As long as the ball doesn’t keep falling off the tee, you can now step up to the box and drive the ball in just about any direction you want, with the exception of straight down. Works great for golf, but how can such an unstable joint work in our body? Simple. The glenohumeral joint can only be so amazing with the help of the scapulothoracic joint.
The glenohumeral joint is the MVP of our shoulder complex. It’s flashy, makes the big plays, and scores all the points. The GHJ joint is the single most mobile joint in the body. But, thanks to the laws of physics, mobility exists at the expense of stability. Picture a golf tee and a golf ball – this is the age-old analogy that best describes the dimensions of the GHJ joint. When the tee is set just right, the ball can sit perfectly centered in the shallow support of the tee. As long as the ball doesn’t keep falling off the tee, you can now step up to the box and drive the ball in just about any direction you want, with the exception of straight down. Works great for golf, but how can such an unstable joint work in our body? Simple. The glenohumeral joint can only be so amazing with the help of the scapulothoracic joint.
The scapulothoracic joint is the bread to our PB&J, our Phil Jackson to Jordan and Pippen, and the fuel to Cheech and Chong’s fire (or should I say smoke?). Without the scapulothoracic joint, the glenohumeral joint would be rendered useless. The relationship between these two joints is all too often overlooked when addressing the shoulder as focus is instead shifted to the ball and socket (alone) or the scapula (alone). The coupling of the GHJ and STJ effectively links the arm to the thoracic vertebrae meaning dysfunction of the spine can compromise the shoulder – and vice versa.
The Scapula and Stability
 Here’s how the dots connect. Starting from midline, the thoracic spine forms a column from which twelve ribs attach. These ribs wrap around in a barrel-like fashion, creating the rib cage. Consider the thoracic vertebrae the foundation under a building and the ribs the floors sitting on top. The triangular-shaped scapula sits on top of the ribs, just as a rug would lay flat on a floor.
Here’s how the dots connect. Starting from midline, the thoracic spine forms a column from which twelve ribs attach. These ribs wrap around in a barrel-like fashion, creating the rib cage. Consider the thoracic vertebrae the foundation under a building and the ribs the floors sitting on top. The triangular-shaped scapula sits on top of the ribs, just as a rug would lay flat on a floor.
At rest, the superior border of the scapula runs horizontally from shoulder to spine and then turns down at a ninety-degree angle continuing parallel to the spine as the medial border of the scapula. A little more than midway down the spine the scapula turns up, becoming the lateral border as it heads up and out toward the armpit where it meets the superior border to complete the triangle. This junction of the superior and lateral border creates a projection called the glenoid fossa, which you know as the socket. The glenoid holds the ball, which is the rounded end of the humerus bone, to form the glenohumeral joint.
Say we are moving furniture into a building. We require that a solid foundation provide the base for our building. Then, flooring would need to be installed so that we can lay down a rug. Only after these steps are taken – in this order – furnishings can be brought in. Similarly, we must ensure a stable spine and ribcage for the scapula to sit on so that it can in turn be a reliable support for the arm. Stability at each and every link along this kinetic chain is necessary for function as a whole. Without Jordan bringing his A-game, Pippen performing to full potential, and Phil Jackson calling all the right plays there is no three-peat championship for the Chicago Bulls.
The Muscles Involved With the Shoulder Complex
 The good news is that we are much more like the Bulls than a building. While we ideally have “good bones” like a building, that’s where the similarities end. We are more than a skeleton. We don’t sit idly. We don’t break and not bend. We are dynamic. We act and react. We can take our sturdy foundations and move them in all kinds of ways, producing amazing feats – like drilling the game winning three-pointer at the buzzer. But, as important as our bones are, we can only control what they do with our muscles. When it comes to operating the shoulder complex, the rotator cuff, scapular stabilizers, and core muscles are in charge. Without these muscles, we are just an idle structure.
The good news is that we are much more like the Bulls than a building. While we ideally have “good bones” like a building, that’s where the similarities end. We are more than a skeleton. We don’t sit idly. We don’t break and not bend. We are dynamic. We act and react. We can take our sturdy foundations and move them in all kinds of ways, producing amazing feats – like drilling the game winning three-pointer at the buzzer. But, as important as our bones are, we can only control what they do with our muscles. When it comes to operating the shoulder complex, the rotator cuff, scapular stabilizers, and core muscles are in charge. Without these muscles, we are just an idle structure.
Stability of the glenohumeral and scapulothoracic joints occurs in a specific order. First, the thoracic spine moves (or doesn’t) thanks to our core muscles. Then, our scapula is anchored to the spine and ribcage via several different stabilizing muscles. Lastly, the rotator cuff travels from the surface of the scapula, crossing the glenohumeral joint to hold the ball into the socket. Centered around the scapula, these three groups of muscles work together as a kinetic chain connecting the core to our upper extremity. The scapulothoracic joint, as a result, is the key to the shoulder. Insufficient stability of the STJ is the main ingredient in the recipe for disaster – and not just at the shoulder. Inability to control the scapula can lead to neck pain and headaches. Weakness of the shoulder blade not only decreases the ability for the arm to function, but it can also bring us down, literally. A slouched posture and overextended spine can both result from weakness at the scapulothoracic joint.
Control your scapulothoracic joint, and you control your ability to make gains with strength and power, abolish or avoid pain and dysfunction, and most importantly, take a huge stride toward mastering the complexity of human performance. Controlling your STJ is easy, and I’ll show you how. Next time.

Total Physical Therapy & Lauren Beasley changed my life. I am enormously grateful. I came to TPT after “resting” a chronic hip injury for 14 months based on my doctor’s advice. The injury stagnated and would not resolve itself. From the initial phone consultation, Lauren Beasley of Total-PT was engaged, enthusiastic, and confident she could improve the situation and get me back to running and normal fitness activity. Having now successfully completed my physical therapy program, I am now back to my pre-injury activities and completely thrilled with the entire experience. There is no substitute for the personal, one-to-one approach Total-PT takes to it’s patients. The therapist is not circulating from one patient to another during your session. You are the sole focus for that hour. The exercises and techniques are tailored to you, how you are feeling that day/week, and what the right next progression is. Lauren Beasley was excellent at explaining the reasons for the therapy she recommended, how it relates to anatomy and biomechanics. She was also available and happy to chat or text between sessions if something came up. It is true personal service, and done with a great attitude. I would recommend Total Physical Therapy to anyone who is committed to resolving an injury through exercise and improving their strength, mobility and flexibility.

Thanks Lauren! Christian just called. He set a personal record tonight in the 400 meter at the NYC armory. He ran a 50.6 and got a silver medal. He was the only Seton Hall Prep runner to qualify for the Eastern States later this month. All this with no practice in the last three weeks! He thanked God first, and you second!
Much appreciated!

Here’s Lauren Beasley’s follow-up article as featured in Breaking Muscle
We need stability in much the same way that we need air. We need to supply oxygen in the right amounts, at the right times, and according to the demand. It’s a simple supply-demand relationship and the same goes for stability. For years, the core muscles (read: abs) have been the focus of stability training and with good reason. The muscles traditionally referred to as “the core” provide a working surface for our extremities to push off of, which is crucial for any kind of movement, from throwing the game-winning touchdown pass to signing an autograph after the victory. You’d be hard pressed to find someone with a good argument for not training core stability.
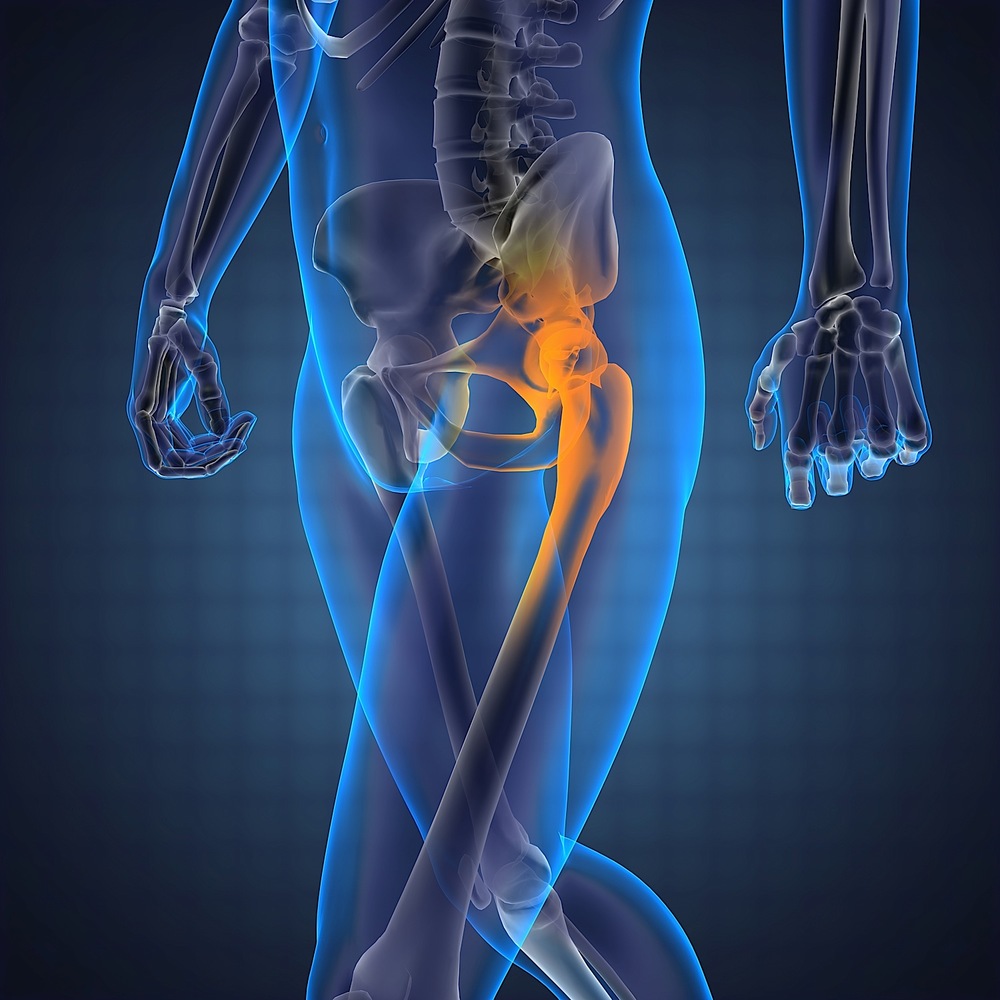
 But there’s more to the story. The core is where we generate, absorb, and transfer forces to and from our extremities, which means we need to focus on stabilizing the connection between extremity and core. Enter the hip.
But there’s more to the story. The core is where we generate, absorb, and transfer forces to and from our extremities, which means we need to focus on stabilizing the connection between extremity and core. Enter the hip.
In my last article, I shared knowledge that came from years of seminars, textbooks, mentorships, and trouble-shooting all kinds of injuries. I revealed that hip instability is the common thread of so many problems – from back pain to shin splints – and sub-par hip performance is far more common than you might think. But unless you’re in a serious state of denial, admitting that your hip isn’t working so well is not the hard part – fixing it is. So, let’s make this simple. I’m going to break fixing your hips down into five steps:
Step #1: Deep Tissue Mobility
I know, you expected strength and stability drills, but before you ask your muscles to work, you should probably make sure they are able to work. Foam rolling and lacrosse ball mobility drills have become all the rage, but while “everyone’s doing it” is a good enough reason to get most people on the bandwagon, understanding the purpose and value of these drills will help prioritize when and where you should spend time suffering through deep tissue mobility work.
When a muscle is tight, range of motion can be compromised. Lack of range of motion causes changes in movement patterns that limit quality of performance and ultimately create injury risk. A tight muscle is a weak muscle. An overstretched or long muscle is also a weak muscle. This conundrum is known as the length-tension relationship. In short, this rule says that a muscle must be at mid-length (or on a slight stretch, to be exact) to generate optimal force. If a muscle contracts by shortening, how can the muscle generate force if it is already shortened? This concept applies not only to overall length of muscles, but to isolated units within a muscle.

We know that several muscles play an intricate role in supporting the hip joint, but I’m going to play favorites and pick on the gluteus medius. Not just because it is notoriously tight, but because this is the most common source of breakdown I come across in the clinic. And the glut med is no job for a foam roller – too close for missiles, Mav, better switch to guns. Due to its smaller surface area, the lacrosse ball is the perfect tool to dig into the lateral hip and provide enough pressure to release the fibers. Spend a few minutes on each side, and consider your glutes ready for action.
Step #2: Isolated Strengthening
Turns out, there is a purpose for those wimpy isolation exercises that have been shunned by the fitness world in lieu of functional training. (Don’t worry – we’ll get to that, too.) After step one, you’ve smashed, mashed, and rolled your hip fibers into prime shape for work, and while they can now create a stronger contraction, they are clearly still weak. This second step is not a quick fix and requires some good old-fashioned hard work. Cue: targeted, remedial strengthening.
Before I step into the lion’s den by singling out some exercises, let’s get a few things straight. First, I have read many studies examining the best way to elicit hip muscle activity and there are a lot of conflicting results. Regardless of the exercise, a major factor in the effectiveness of targeting a specific muscle is cuing and awareness. In other words, if a person tries to squeeze their glutes during an activity, then the glutes are more active. Second, if a person has weak glutes, then pretty much any method of targeting glute strength will do, as anything is better than nothing. Lastly, anything is better than nothing also applies to compliance. If an athlete isn’t going to do the exercise then it’s not very effective, is it? So let’s keep it simple and easy to perform.
While this overview of hip strengthening methods is far from comprehensive, no list of lateral hip exercises would be complete without side-lying abduction. After all, this is the primary “action” of the glute med when the muscle fibers concentrically contract. Additionally, side planking is an excellent way to isometrically fire the glute med as the lateral hip muscles keep you off of the ground. Want to get fancy? Hold a side plank and perform abduction with the non-weight bearing leg.
Step #3: Functional Strengthening
 Moving right along! Your glute med is now willing and able to work, so the important focus now becomes retraining this muscle to work functionally. In weight bearing, the glute med must fire to stabilize the pelvis, mainly in unilateral stance. Therefore, I recommend targeting the glute med in weight bearing with focus on double- and single-limb stance.
Moving right along! Your glute med is now willing and able to work, so the important focus now becomes retraining this muscle to work functionally. In weight bearing, the glute med must fire to stabilize the pelvis, mainly in unilateral stance. Therefore, I recommend targeting the glute med in weight bearing with focus on double- and single-limb stance.
A simple way to ensure the glute med is firing as you weight bear is to use a resistance band around the ankles or knees while walking. Forward, backwards, laterally – whatever method suits your mood. Lateral step-ups and single-leg Romanian deadlifts also work well to functionally train the glute med.
Step #4: Dynamic Stabilizing
Continuing along this progression, it is now time to make sure we can supply hip stability in the right amount, at the right times (just like oxygen). Plyometric work such as speed skaters and single leg work in the form of broad jumps or box jumps require the glute med to stabilize the pelvis during more dynamic activity. This is challenging, but struggling with this stage is necessary in order to carry over good movement patterns established in simple, controlled activities to more unpredictable situations.
Step #5: Skill
Here’s the fun part. How you choose to use and challenge your shiny new hip stability is up to you. Your sport will guide the next steps in training your hip to ensure your stability is up to par for the specific demands you place on your body. Remember, breaking down complex skills into their smaller parts is crucial to successful performance. Perfect practice makes perfect.
That’s it. A systematic approach to tackle movement dysfunction. Using this logic, now you can apply your own tried and true techniques. (Spoiler alert: this also works pretty well for our other core-extremity connector, the shoulder.)
